
It’s Breast Cancer Awareness month and you might be thinking of your annual women’s health checks. If you haven’t done a mammogram in Hong Kong before and don’t know where to start, here’s everything you need to know about breast cancer screening and prevention. We hope you stay in the “pink” of health!
If you haven’t noticed already, October is covered in pink. This is the only month when this rosy hue ceases to be just a colour; it also becomes a verb. Since 1985, October has been marked as Breast Cancer Awareness Month.
“Pinktober” is also synonymous with women in the 40 to 70 age group scheduling their annual mammograms. The idea behind advocating mammography after a certain age is to catch the disease earlier and help doctors save more lives. We analyse the benefits and the limitations of universal mammography programmes and if the results are as rosy as expected. If you are trying to make sense of breast cancer screening methods, this is your guide to understanding mammograms.
Read More: Know Your Body – Learn How To Correctly Perform A Breast Self-Exam

What To Expect From A Mammogram
As with many women’s health checks, the pre-mammogram dread is only natural. When you think of round breasts and flat, cold plates, the mental image you may conjure up is of being in a panini press. It is uncomfortable and the experience is a tad rougher for women with smaller, sensitive and denser breasts but it’s not unbearable and it’s over pretty quickly. Mammograms are an outpatient department (OPD) affair. You can walk in and out of a scheduled appointment earlier than you do at a nail salon.
Don’t dab deodorant, perfume, talcum or any lotion on your boobs or pits that day – foreign particles can mess with the x-ray and show up as calcification on the film (basically, calcification is an indication of an infection, cyst or injury to the breast tissue). Inside the clinic, you strip to the waist, remove neck jewellery and allow the technician to squish your boobs in the metal mammography box. A couple of images per breast later (take a deep breath) and you’re on your way home.
After the mammogram, the radiologist looks out for any tiny white spots called calcifications, lumpy tumours or any suspicious signs of malignancy. It is important that women know and understand that not all calcifications (calcium deposits) and tumours spotted in mammograms are cancerous. A follow-up diagnostic scan or a tissue biopsy can confirm that, and in roughly 80% of cases, the biopsy comes back negative (thankfully!) so always wait for this result before considering next steps.
Read More: Where To Find Counsellors, Psychologists And Therapists In Hong Kong

Mammograms Versus Breast Ultrasounds
The difference between mammography and sonography (of the breast) lies in the roles these technologies are designed for. A mammogram is an effective tool for screening any abnormalities with your breasts even when you don’t have any symptoms. It takes images of the deep breast tissue but it can sometimes miss a palpable lump. In that case, ultrasounds, MRIs or CTs are then advised for a more local, in-depth examination.
A breast ultrasound is a diagnostic tool for a localised area of the breast. It’s used for a host of reasons – to evaluate lumps, monitor benign fibroids, assess unusual nipple discharge, and mastitis or recommended for those who should avoid radiation of conventional mams – like pregnant women, women younger than 25, or those with any kind of breast implants.
This should not leave you thinking that ultrasounds are superior to mammograms – both are designed for different purposes and the accuracy of the result can depend a lot on the skillset of the technician.
Understanding Breast Cancer And The Role Of Mammograms In Breast Cancer Screening
Renowned cancer researcher Professor Barnett Kramer at the National Cancer Institute’s Division of Cancer Prevention in the US says that behaviourally, breast cancers fall into three broad types:
Turtles, birds and bears of cancer
- Turtles, as the name suggests, are those cancerous cells that advance so slowly that they never really metastasise enough to pose any danger to one’s life. While you could spot these tumours with a routine mammogram, there is no benefit to early diagnosis as these types of tumours don’t cause harm in the first place.
- Birds are the more life-threatening cancers which grow at a manic pace. Sadly, for those suffering from the disease (and their loved ones), these aren’t usually caught on a routine mammogram because they’ve already spread before detection.
- Bears are the only cancers which are impacted by routine screening. They evolve slowly and are fatal if left untreated. Catching them early on a mammogram can buy time for treatment which can make all the difference.
Want to understand this in more detail? Watch this video explaining the new definitions of cancer by the reputed researcher himself.
Now the issue is that mammography tools at the moment aren’t advanced enough to make a distinction between the turtle, bear or bird types of cancers. And most doctors can never say for certain which tumours are too mild to cause any damage and might even disappear on their own (well-known in testicular cancer). Without knowing how a cancer will progress, the safest course of action is to assume that it falls in a bear category and that it will respond to treatment and then treat it as such.
So a lot of women, with the turtle category of breast cancerous cells, get the “C” diagnosis decades before time. Their world topples and they tailspin into a whirlpool of panic, anxiety and toxic treatments (that come with their own set of side effects) for something that may not have harmed them, if left alone.
Read More: Mental Health In Hong Kong – Let’s Talk About It

Is An Annual Mammogram Recommended?
The jury is still out on that and the answer is fairly complicated. For example, breast cancer screening is considered effective only if it cuts down on the death rates.
There are plenty of studies that suggest that annual screenings have not lowered death rates of breast cancer. A large-scale Dutch study, published in the British Medical Journal, claimed that 13 years after universal screening started in The Netherlands, the incidence of the deadly, advanced cancers remained “essentially unchanged”. A review by the Swiss Medical Body published in the New England Journal of Medicine states that for every 1,000 women exposed to an annual mammogram, only one additional life is saved. It even went on to boldly recommend that their country stop the annual breast cancer screening for women and that routine mammography “is hard to justify”. The statement understandably caused a prickly debate but the medical body stood its ground.
And yet, there are other medical boards and governments that recommend breast cancer screening. The American Cancer Society recognises the role of mammograms in the early detection of breast cancer and has different guidelines for women of average and high risk. In the US, there is an organisation, the United States Preventive Services Task Force (USPSTF), that is made up of doctors and disease experts who look at research on the best way to prevent diseases and make recommendations on how doctors can help patients avoid diseases or find them early. The USPSTF recommends that women who are 50 to 74 years old and are at average risk for breast cancer get a mammogram every two years (this is currently being reviewed and may change). There are similar guidelines by the Cancer Research Institute and the NHS in the UK. The NHS clearly outlines the risks and limitations of mammograms but recommends a screening once in three years for women between 50 and 71 years.
Read More: Where To Buy Supplements in Hong Kong For The Family
Breast Cancer Incidence In Hong Kong
Statistics from the Hong Kong Breast Cancer Foundation show that breast cancer has become the most common cancer affecting women in Hong Kong since 1994.
- About 12 women are diagnosed with breast cancer every day.
- The lifetime breast cancer risk for females is 1 in every 14.
- The median age of breast cancer patients in Hong Kong is 58 years, compared to 63 in the United States.
- Though the majority of women diagnosed with breast cancer are between 40 to 59 years, the youngest case was below 25 years old.
Read More: Best Child Psychologists, Therapists And Counsellors In Hong Kong
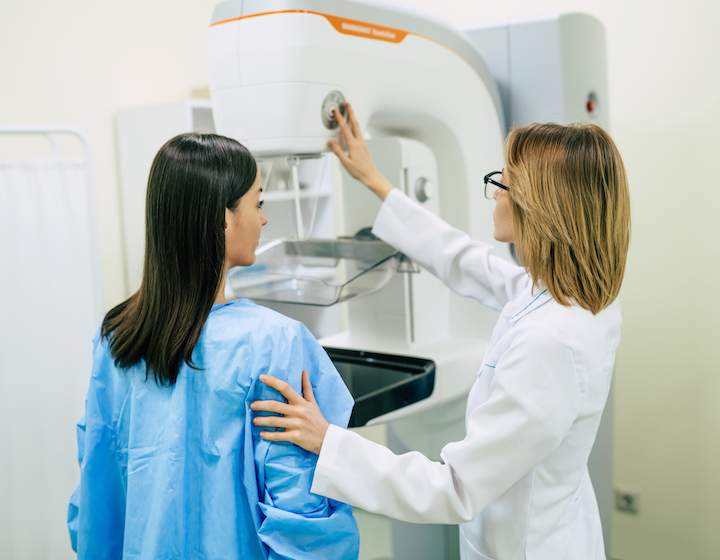
Annual Mammograms And Breast Cancer Screening: The Official Guidelines For Hong Kong
So what are the guidelines in the 852? Starting in September of 2021, the Breast Cancer Screening Pilot Programme was rolled out to provide screening services for eligible women over a period of two years. The aim is to detect early breast cancer in women before any symptoms of breast cancer appear so treatment is carried out at the earliest.
This is based on the revised recommendations of the Cancer Expert Working Group on Cancer Prevention and Screening (CEWG) of the Cancer Coordinating Committee. This risk-based approach for breast cancer screening is to consider mammography screening every two years for women aged between 44 and 69 years with certain combinations of personalised risk factors. Want to understand your own risk profile? Read the details here.
Women in Hong Kong are advised to carry out routine breast self-examinations so they become familiar with what’s normal for them at a certain point in their menstrual cycle and bring up any noticeable changes to their doctor’s attention.
Read More: Practical Period Advice To Share With Your Teenage Daughters

So What’s Best For Your Breasts?
Mammograms are not perfect and unfortunately, they do miss some cancers. Also, screenings often lead to the very real danger of overdiagnosis, i.e., getting diagnosed with cancer that never would have caused any problems. After an initial screening (even if it’s a positive), sometimes a woman will need more tests to find out if something found on a mammogram is or is not cancer. It’s important that women who are getting mammograms know what to expect. They should also understand the benefits and limitations of breast cancer screening.
When it comes to cancer, no one is invincible. It is important to have a meaningful conversation with your doctor and chalk out a customised risk assessment plan after taking your lifestyle and medical history into account. Doctors should present clear data on the benefits and limitations of mammography and the burden of overdiagnosis. So, instead of being population-based, regular mammography should be an individual choice based on age, family history or the presence of BRCA1 and BRCA2 genes (this video may help you make your decision). Regardless of the risk level, all women need to do a regular self-exam to feel for lumps, bumps or any visible changes with your breasts.
We’re thinking pink this October and want to do our bit to spread awareness about breast cancer. For further information, contact the Hong Kong Breast Cancer Foundation (HKBCF).
Read More: Where To Donate Blood In Hong Kong
Editor’s Note: “Breast Cancer Awareness Month: Understanding Mammograms, Screening And Prevention” was most recently updated in October 2025 by Sassy Mama. Special thanks to Nikita Mishra for her contribution.
 View All
View All










 View All
View All




 View All
View All

 View All
View All















