
How to get active again after giving birth.
New mums have so many questions about exercising after your pregnancy. Is it safe? When can you start? Is leaking normal? Will you ever shift that mummy tummy? Can you go back to your pre-pregnancy workout routine?
You probably have a ton more! Unfortunately, it can be hard to find the right answers and to know if you’re on the right track. So let’s equip you with the tools to start feeling yourself again!
There’s a lot of ground to cover, so jump to what you need to know:
Before You Begin
0 – 6 Weeks After Delivery
7 – 18 Weeks After Delivery
19 – 42 Weeks After Delivery
C-Section
Diastasis Recti
Pelvic Organ Prolapse
Incontinence
Vaginal Tearing
Mind And Body
Read more: Pre And Postnatal Fitness Part 1: Safe Exercise For The First Trimester
Before You Begin
- Your postpartum recovery is going to take longer than you think. Carrying a baby in your body for months and giving birth creates huge psychological and physiological changes in your body. Don’t put any pressure on yourself to spring back into shape immediately. Instead, when recovering, take things slowly and progressively.
- Your pregnancy and birth experience was totally unique. Some of you will have had a planned c-section, an unplanned c-section and some a vaginal birth. Some of you will have given birth for the first time, while others may be on your third or fourth child. These and a myriad of other factors mean you will need to recover, rebuild and reinforce your postpartum bodies in different ways. There is no one-size-fits-all magic exercise plan. And there is no “normal” postpartum experience or fixed timeline that you should expect to follow for your recovery.
- If you continue to have concerns that are not addressed in this guide, you should absolutely seek professional help as soon as possible. You are not alone in this journey. There are doctors, pelvic health physiotherapists, psychologists and coaches who can help you. And if you’d like to get more specific information about your condition and your postpartum goals, please don’t hesitate to get in touch. I am always available to chat!

Slow and Steady
When exercising after your pregnancy it pays to take things slowly. Don’t expect to jump back into your old routine after your first six-week check-up with your doctor. I know it can be hard to hear, especially if you are dying to get back into your running habit or you want to get rid of your tummy as soon as possible. But trust in the process.
Your pregnancy has created profound muscular, postural, internal, hormonal and emotional changes in your body. You’ll need time to recover and rebuild. Think of this period like a long term investment in your health. Take the time to build strong foundations. You will reduce your chance of injury and you will reduce the impact of common postpartum issues like incontinence.
Below is a rough guide to the kinds of light exercises I would recommend doing in the weeks following your birth experience. However, as I said earlier, every woman’s experience and recovery process is individual, and some of you will recover faster than others. Do not feel that this is a timetable that must be followed. Listen to your body and if you are experiencing pain or discomfort during the exercises, stop, rest and, if necessary, consult a medical professional.
0 – 6 Weeks After Delivery
Rest and recovery is key during this phase. I know this can be hard to prioritise if you’re trying to adjust to your new role as a mum and if you are feeling stressed and sore. But listen to your body and don’t be afraid to ask for help.
If you are feeling mobile, pain-free and your doctor has given you the green light, you can start to incorporate breathing exercises, walking short distances, as well as doing some light stretching and gentle mobility work. Keep in mind that this timeline will be a couple of weeks longer for c-section mamas. And don’t be disheartened if you need a little longer than six weeks. It’s not a magic number and rushing will not help you recover faster.
You might be tempted to skip the breathing exercises and go straight to walking and mobility work. But breathing exercises will help improve your patterns and are an absolutely key component of postpartum recovery. You are aiming to get your entire core in sync and working together with every inhale and exhale you take. This means syncing up and engaging your diaphragm, pelvic floor, back muscles and abdominal wall. And it’s not as easy as it sounds. I’ve spent months working with clients to reconnect and “feel” their core again.

So why is this so important? Because your core is the foundation for the support and stability of every moving part of your body. Get this right and you’ll set yourself up for more challenging movements and exercises later on. Ignore your core and you may expose yourself to injuries and exacerbate existing postnatal conditions.

In terms of mobility and stretching exercises in your first few weeks, knee rolls and pelvic tilts are good (shown above) movements to incorporate (only if you are feeling well enough to do them).
Read more: The Fourth Trimester: What To Expect When You’re No Longer Expecting
7 – 18 Weeks After Delivery
You will normally have a doctor’s assessment around your 6th to 8th week postpartum. If you have been cleared to exercise by your medical practitioner, you can start to think about adding specific exercises to restore your core and pelvic floor, as well as building on functional exercises that complement everyday movements like picking up your baby and getting up from the sofa. But start slow and light and be cautious to begin with. If you have not yet been cleared to exercise, don’t worry. Rest and recover until you are well enough.

Simple functional exercises such as box squats (above) and seated single arm cable rows (below) can be added at this stage. Even if you were using dumbbells and kettlebells before and during your pregnancy, stick to bodyweight exercises initially. Work your way up gradually only if you are not in pain and do not experience any discomfort in your core and pelvic floor. Don’t go for more than 2 to 3 sets of 8 to 12 reps.

In addition, you can begin exercises that recruit your core. A strong core will help you a lot as a mum. It will improve your posture, you will find it easier to carry baby and it will help you recover from diastasis recti. When working your core, stay away from heavy front-loading exercises like planks, which might put too much pressure on your abdominal wall. And stay away from advanced exercises like leg lifts, sit-ups, crunches and flutter kicks, which may put too much strain on your core and pelvic floor.

Instead, practice exercises like the bird dog (modify to your level, beginner – leg slide; intermediate – legs only; advanced – arms and legs; shown in order below), the kneeling pallof press and heel slides (above).
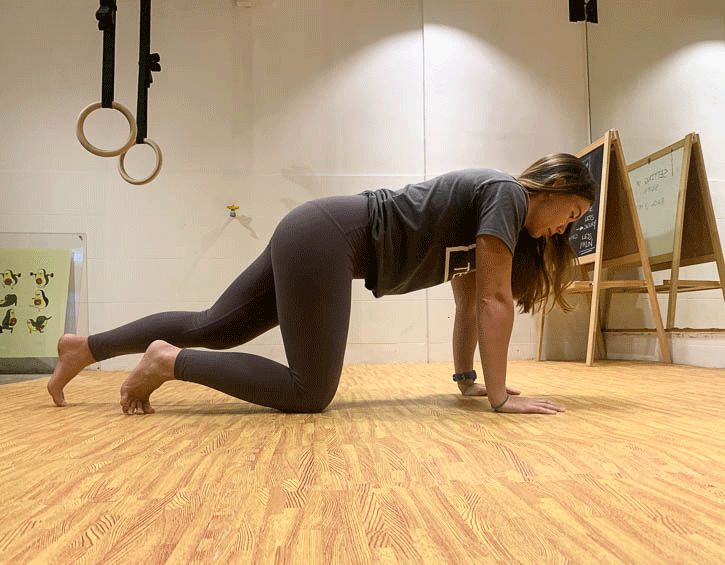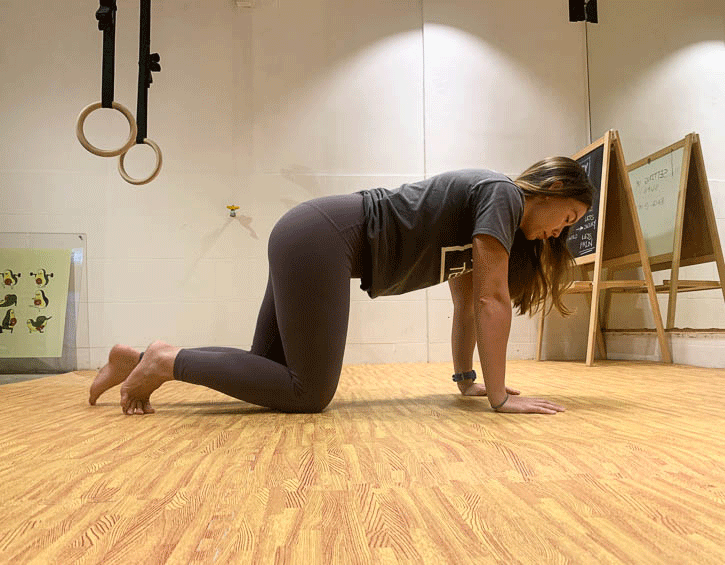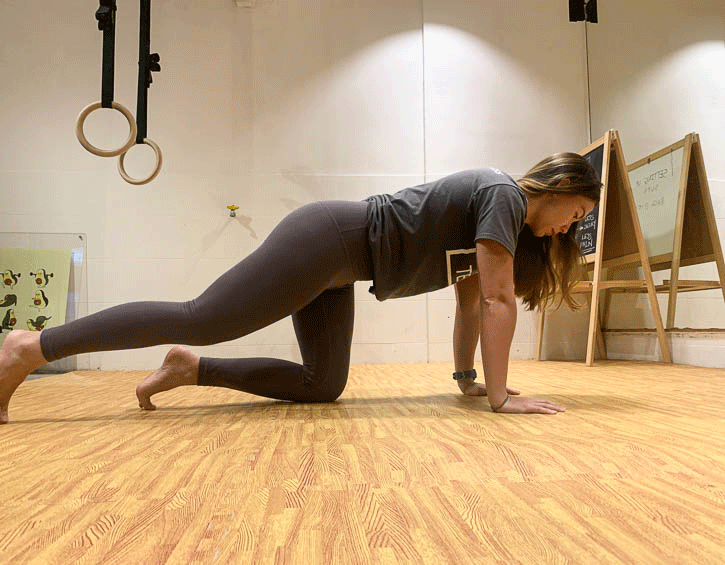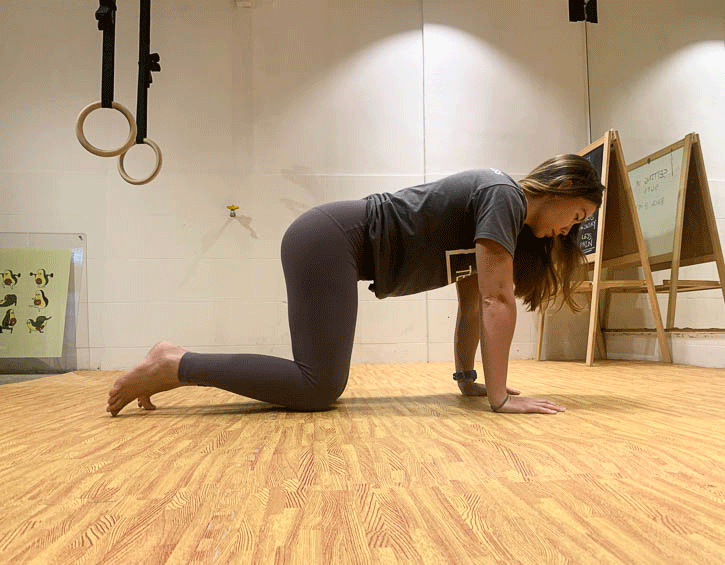
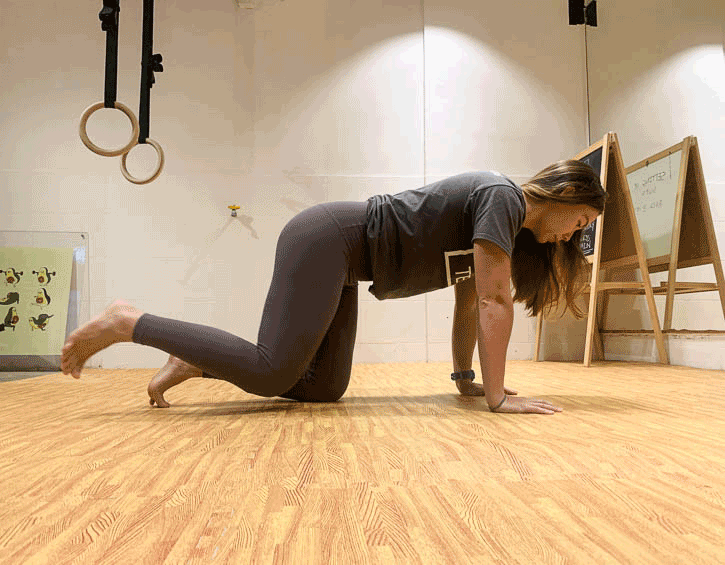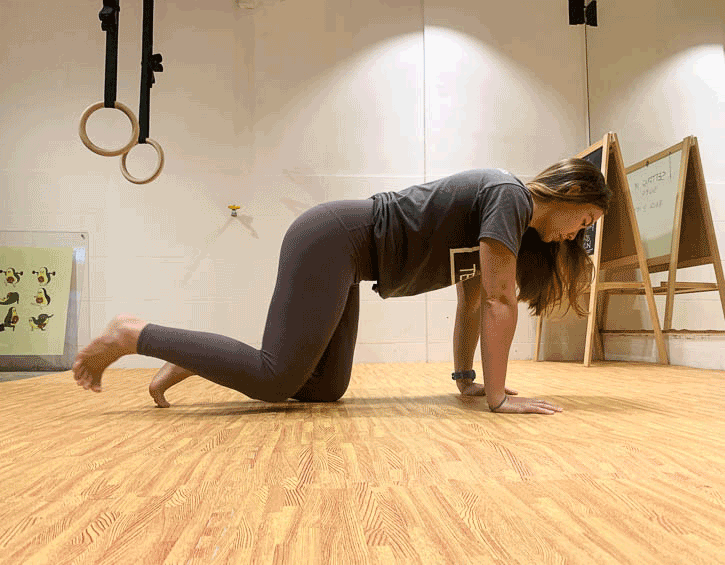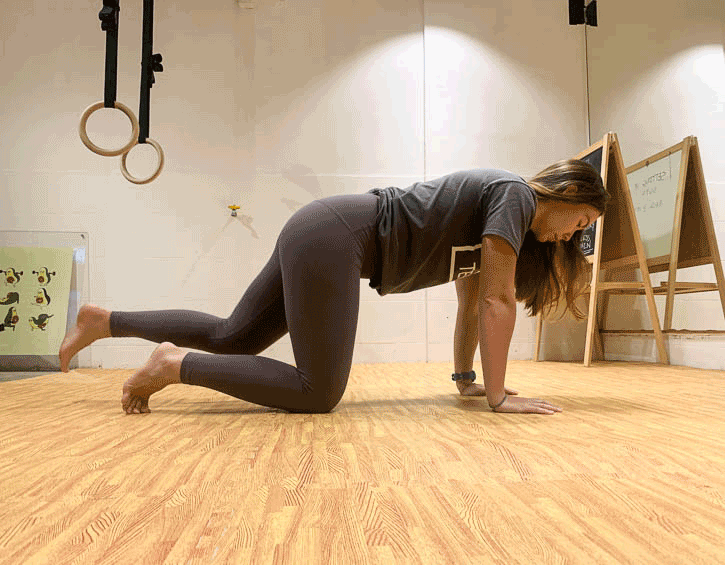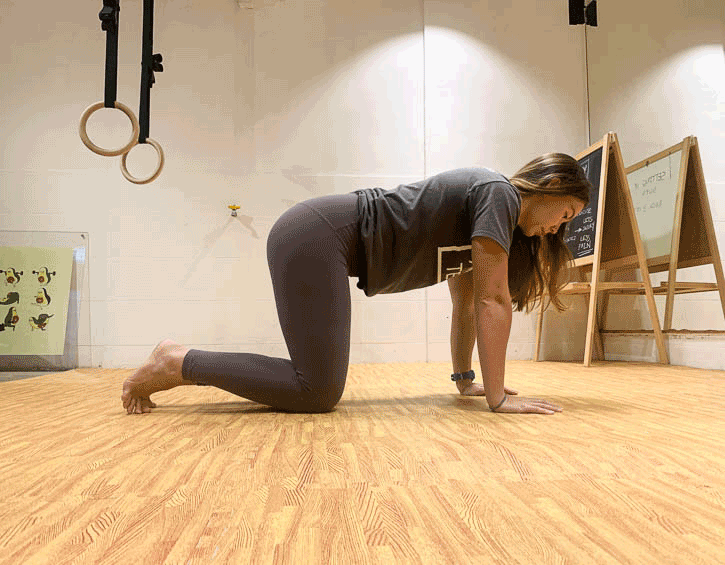
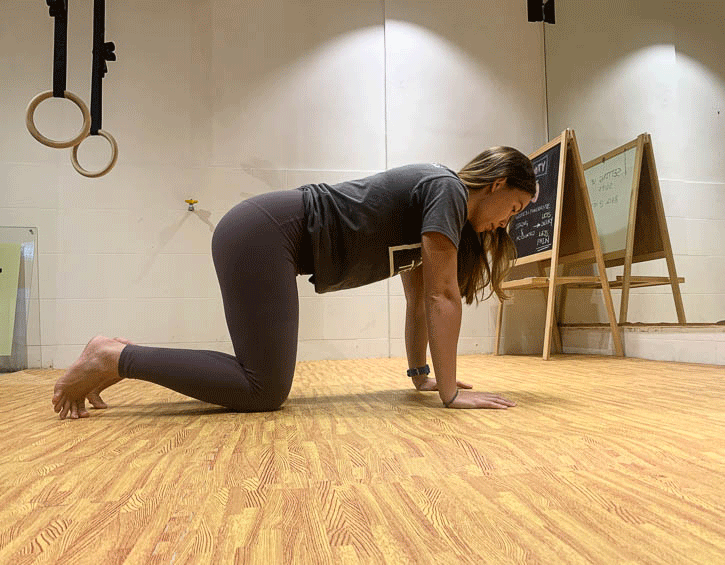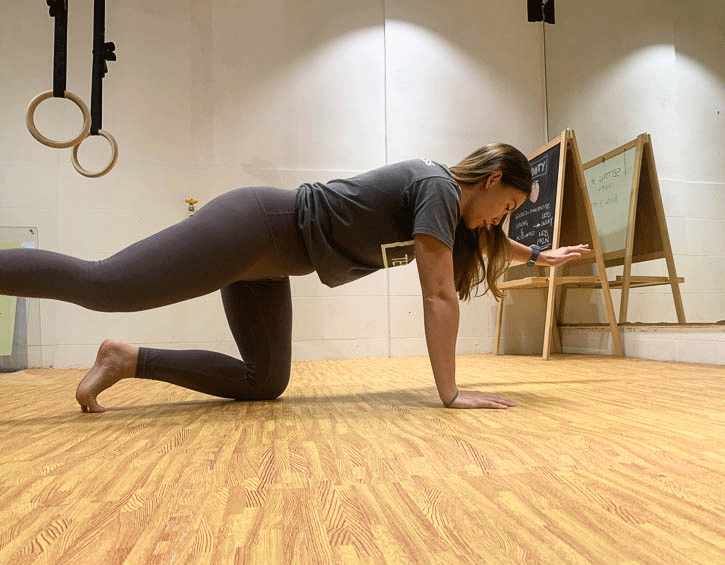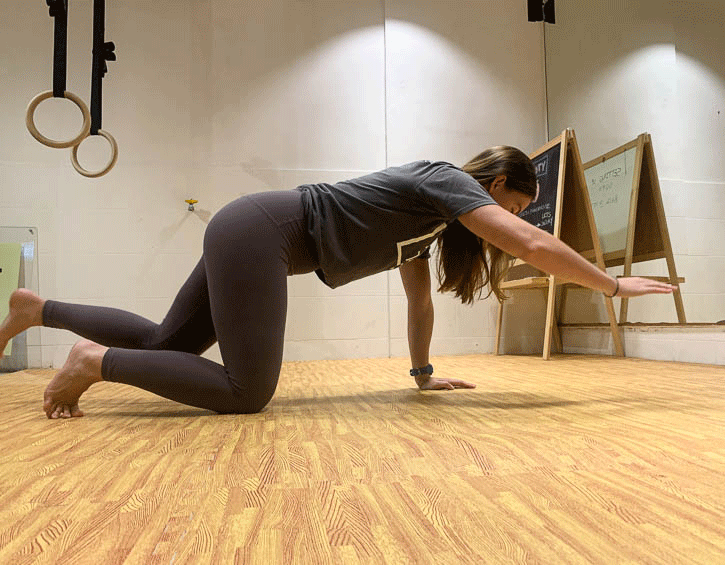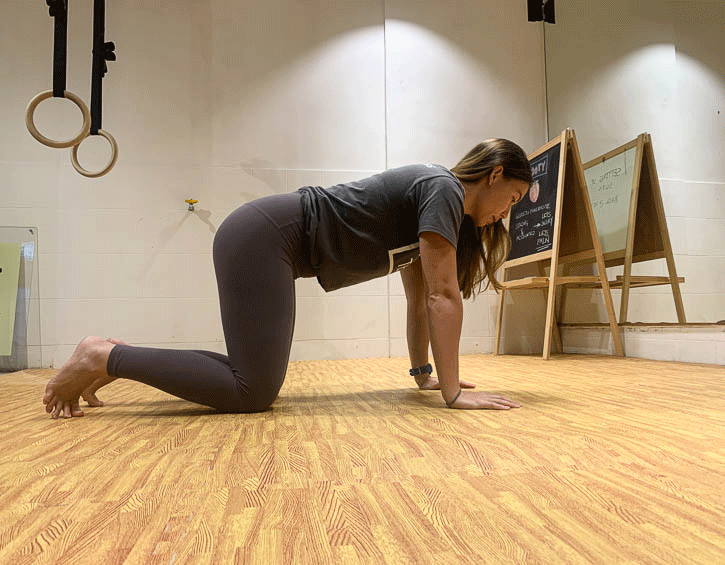
Mix these up so that you engage your core in a variety of positions, like supine, kneeling and on your side, as these will give you the best all-round workout.
Finally, you can also transition from light walks to moderate cardio to improve your aerobic fitness (but keep the intensity low). Avoid high-impact cardio exercises, which put too much pressure on your pelvic floor. A good rule of thumb is to make sure that you have enough breath to have a conversation with a friend throughout the exercise. You don’t want to be exercising so hard that you are breathless. You also don’t need to go past 45 to 60 minutes per session.
It’s natural to want to do more at this stage and you might be tempted to add weight, exercise more often and start doing more intense kinds of exercise. Again, proceed with care, and be careful not to push it too hard too early. A useful tip is to follow the 10% rule.
The 10% rule works like this – there are three ways you can exercise harder:
- Frequency – increasing how often you exercise
- Intensity – increasing how much you exert yourself in each exercise session
- Time – increasing the length of each exercise session
The 10% rule means that you can ONLY choose one of these options and increase it by 10% each week. For example, if you start with a gentle 20-minute walk on week seven (and you feel okay), you can add 10% in week eight by walking for an additional two minutes.
During this phase, it’s also important to continue working on your posture and your breathing. Think about exhaling on the more difficult part of the exercise, like when you’re standing up from the bottom of a squat. Why is this important? Because when you exhale correctly your pelvic floor lifts and your abdominal wall contracts, and this movement protects your spine and internal organs. I want to equip you with this skill so that when you need to lift your baby you won’t injure yourself in the process.
19 – 42 Weeks After Delivery
This is where you can begin to reinforce the hard work you have put into rebuilding your core and pelvic floor. But don’t forget to keep working on your breathing exercises too.
Carefully increase the volume of aerobic exercise. Don’t go all out with a 5km run. Instead, start with a more mild combination of alternating walking with a short jog. This will put much less strain on your pelvic floor, which you still need to look after at this stage. There are many steps you need to take between leaving the delivery room and going for your first safe run. A good pre and postnatal coach will help you identify and target the areas you need to train in order to get you back on the track or trail. And if you experience any incontinence, stop what you are doing, consult a medical professional and take a few steps back from your training plan.
If you are a crossfitter, or you love high-intensity interval training (HIIT) workouts, you can experiment with returning to some of these activities provided you feel strong and are pain-free. Try to limit these sessions to a maximum of once a week. In addition, be mindful that you will need to modify some of the exercises in the routine. For the time being, stay away from movements that incorporate bouncing and hard landings. Exercises like box jumps and man makers will likely overload your pelvic floor, causing discomfort and symptoms like leaking, which is a big no-no.
Modify push-up style exercises to knee push-ups or front incline push-ups to lessen the load on your abdominal wall. Ideally, if you are really hoping to get back into these kinds of activities, find a postnatal coach who can monitor your progress and make sure that you are proceeding safely to minimise your chances of injury and postnatal complications.
Read more: Back To The Mat: Postnatal Workout Classes In Hong Kong
C-Section
If you’ve had a c-section all the same rules above apply, but I’d suggest taking some extra precautions. Take care to monitor your scar. Only begin exercise when the inflammation has subsided and the scar looks well-healed and ceases to leak. Your rest and recovery period may take a few weeks longer than for a vaginal birth. And that is totally okay.
A c-section is a major surgery involving an incision through multiple layers of tissue. So don’t put pressure on yourself to return to normal function in a few short weeks. Think of a c-section like any other surgical procedure. We all know it can take months or over a year to heal from a surgery like an ACL repair and the recovery time for a c-section should be no different.
You should also be aware that having a c-section does not reduce your chances of pelvic floor dysfunction, because pregnancy (not just birth) puts a massive strain on your pelvic floor. Make sure that if you experience any heaviness and discomfort in your pelvic floor, or if you have problems controlling your bowels and bladder, seek help from a pelvic health physiotherapist.
Diastasis Recti
You might have heard of Diastasis Recti (DR) and you might be confused about how to deal with it, particularly when it comes to exercise. This is no surprise. There is a lot of conflicting information out there about DR and the research on the subject is constantly changing.
If you haven’t heard of DR, here are the basics:
- DR occurs when you experience a loss of intra-abdominal pressure and tension. Simply put, the bulge created by your growing baby stretches the connective tissue that holds your abdominal muscles together. When the tissue (called the linea alba) stretches, your ab muscles are not held as tightly together and in some women the abdominal muscles visibly separate.
It sounds very scary, but DR is a very common postpartum condition. Studies show that the vast majority of women will experience at least a degree of DR after their third trimester. So if you have DR, do not feel like your body is broken. It’s not! There are countless examples of women who have experienced DR and after proper recovery and restoration, have returned to living extremely active lives.

Unfortunately, because each woman is different, there is no magic exercise regime to “cure” DR. However, stay away from the below exercises while you are rebuilding your strength, as they may put additional pressure on the linea alba, and may slow the healing process:
- Crunches
- Sit-Ups
- Leg Raises
- Bicycles
- Knee Tucks
- Front Planks
- Renegade Rows
- Push-Ups
In addition, try and avoid advanced plyometrics like box jumps and two-footed jump rope exercises, as well as HIIT training sessions where these types of exercise are favoured.
You can try regressions of these exercises which put less pressure on your abdominal wall and your pelvic floor. For example, box squats instead of box jumps, incline planks instead of full planks and alternate leg skipping rather than two-footed jump rope exercises.
If you want to check for DR, consult with a women’s health physiotherapist for extra guidance. When you are cleared to exercise, be cautious and listen to signals to stop and seek help. Common symptoms are pain, leaking, pressure on your bladder and rectum, and difficulty breathing.
Pelvic Organ Prolapse
Pelvic Organ Prolapse (POP) occurs when your pelvic floor muscles, fascia and ligaments aren’t able to give enough support to your organs, and they descend through your vaginal cavity. There are different degrees of POP depending on the extent of the drop and different women will experience POP in different ways. However, some common symptoms are heaviness in the pelvis, incontinence, lack of sensation or pain during sex and back pain. If you suspect that you have POP, please see a pelvic health physiotherapist for professional help. They can provide you with a range of solutions to help from rehab exercises to a device called a pessary, which gives you extra support.
As with other common postpartum issues, you should avoid high impact exercises like running and plyometrics, as well as advanced abdominal exercises like crunches. You should also be careful about lifting weights that you find heavy because there is a chance the extra force you exert will bear down on your pelvic floor. Similarly, avoid wide squats and deep squats during your recovery, as these also put a lot of pressure on your pelvic floor.
Learn to re-establish that feeling of connection with your pelvic floor through breathing exercises. Also work on exercises that will help improve your posture, as this contributes to better recruitment of your pelvic floor muscles.
Incontinence
Urinary incontinence isn’t limited to new mums and first-time mums. I’ve met women who have given birth 20 years ago who still suffer from it and think it is normal. But urinary incontinence is not necessarily something you need to live with. You can significantly improve your bowel and bladder control with exercises that encourage recruitment of the correct pelvic muscles. Interestingly, incontinence isn’t always a result of a weak pelvic floor, but can also be the result of an overactive pelvic floor. So learning exercises that give you a greater degree of control over your pelvic floor will give you a greater degree of control over your incontinence. Speak to your postnatal trainer or women’s health physiotherapist about training plans to help with incontinence.
Read more: Pre and Postnatal Fitness Part 2: Safe Second Trimester Exercise
Vaginal Tearing
If you had a vaginal birth, then there is a strong possibility you tore your perineum. Similar to POP, vaginal tearing is classified by your doctor on a degree scale determined by the length and severity of the tear. The longer the tear, the longer your rehabilitation will be before you can return to exercise. If you have vaginal tearing, consult with your doctor or pelvic health physiotherapist to find the best rehab programme. Always stop exercising and get professional help if you experience pain, loss of bladder and bowel control and uncomfortable pressure in your pelvis as a result of vaginal tearing.

Mind And Body
Although I am not a psychologist, I couldn’t finish this guide without at least touching on the mental aspects of your postnatal recovery. A healthy body and a healthy mind go hand in hand. You can’t cultivate one without the other.
Taking the time to assess your postpartum headspace is super important. Pregnancy and birth are not just physically taxing, but also emotionally and mentally taxing too. Almost every mum will feel tired and overwhelmed at some point – especially if their baby is having a tough time sleeping and feeding. And almost every mum will worry about their postpartum body. It’s all normal and you are not alone.
A lot of women experience a condition called “baby blues” for around two weeks after the birth of their baby. Often, this passes by itself. However, if these feelings persist, they can develop into postnatal depression. If this sounds at all relevant to you, seek help with a psychologist who is sensitive to women’s health issues. This is also super important if you are struggling to process a traumatic birth experience weeks after your delivery. Remember that seeking help is not a sign of weakness, but a brave decision! It’s the first step on your road to recovery.
Some Final Thoughts
Postnatal training is a deep and broad subject and there’s no shame in seeking professional help with your recovery. Issues like incontinence and tearing are common but you don’t have to live with them. Although it might feel slow and frustrating at times, stick with your exercise progression. You are investing in you and your health in the long run.
Read more: Pre And Postnatal Fitness Part 3: Safe Third Trimester Exercise
 View All
View All










 View All
View All




 View All
View All

 View All
View All











